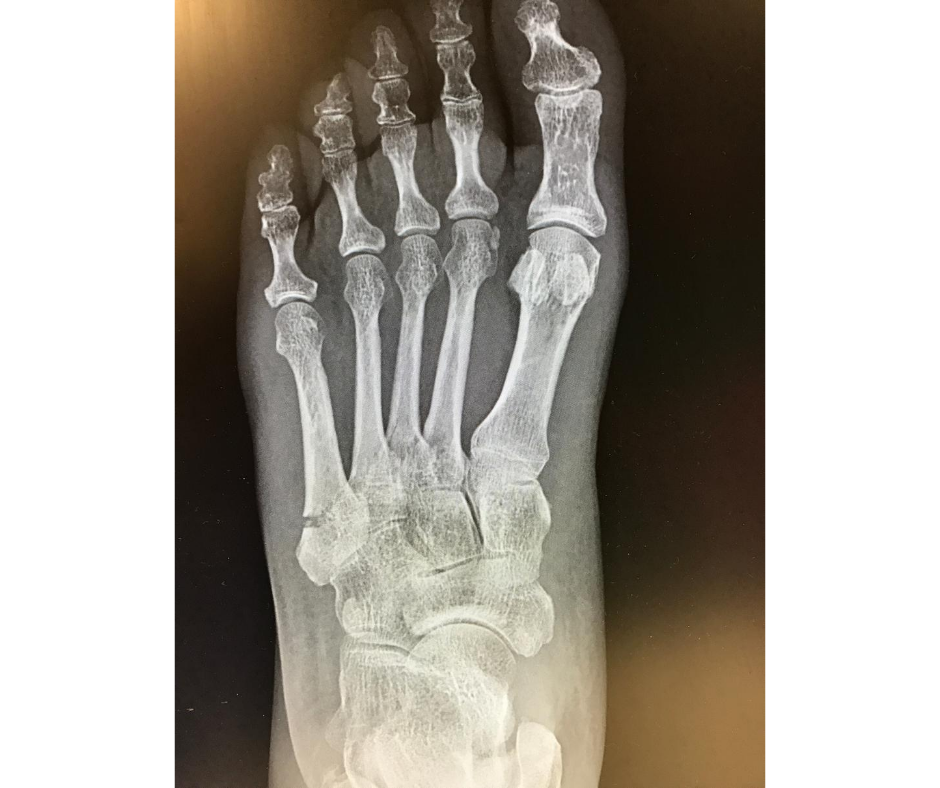
Osteoporosis is a medical conditioning that affects the bones throughout the body, where the bones gradually weaken, become more fragile, and are more vulnerable to breaking from even minor bumps or trauma. Sustaining a fracture (broken bone) to the lower limbs can greatly affect mobility, independence and quality of life – with people aged over 45 years reporting a poorer general health status when living with osteoporosis, compared to those without.
Osteoporosis is a medical conditioning that affects the bones throughout the body, where the bones gradually weaken, become more fragile, and are more vulnerable to breaking from even minor bumps or trauma. Sustaining a fracture (broken bone) to the lower limbs can greatly affect mobility, independence and quality of life – with people aged over 45 years reporting a poorer general health status when living with osteoporosis, compared to those without.
Here in Australia, it is estimated that up to 2.2 million of us are affected by osteoporosis, with 20,000 hip fractures every year – a statistic that appears to be increasing by 40% every decade. Unfortunately, many people don’t become diagnosed until the moment they sustain a fracture, meaning they don’t know to take the right preventative measures before any injury occurs.
What Causes Osteoporosis?
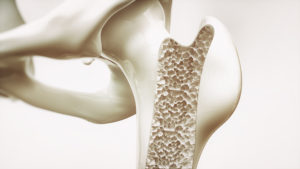 Osteoporosis occurs when you lose bone density much faster than what is considered to be ‘normal’ with ageing. There are a number of risk factors, with some affecting the strength of the bones, and others reducing the quantity of bone tissue that our bodies make and repair.
Osteoporosis occurs when you lose bone density much faster than what is considered to be ‘normal’ with ageing. There are a number of risk factors, with some affecting the strength of the bones, and others reducing the quantity of bone tissue that our bodies make and repair.
Remember, bone is a living tissue, and throughout our lives, new bone is regularly replacing older bone. As we age, the function of many of our bodily processes gradually declines, and our bone-building cells are no exception. Factors that may increase your risk of osteoporosis include:
- Age – after the age of 50, our risk of osteoporosis increases significantly
- Smoking – as it slows down the cells that build bone in the body
- Female gender – women have a higher risk due to both hormonal changes (particularly estrogen which helps promote strong bones, which is lost during menopause) and the predisposition to have smaller bones
- Lower body weight – particularly having a BMI of 19 or less
- Low physical activity levels – as regular exercise helps promote bone strength
- Poor diet – particularly one that is lacking in vitamin D and calcium
- Medical conditions – like arthritis, Crohn’s disease and hyperthyroidism
- Excess alcohol consumption – as it affects the bone-building cells
- Certain medications – like steroids, anti-epileptic treatments, and some cancer treatments
- Family history – you are more likely to have osteoporosis if your family members did too
- History of fractures – research shows that if you’ve broken a bone previously, you’re 2-3 times more likely to break another
Osteoporosis & Osteopenia – What’s The Difference?
Before you have a diagnosis of osteoporosis, you may receive a diagnosis of osteopenia. This means that your bone density has decreased, but is not low enough to be classified as ‘osteoporosis’. In this case, you still need to take extra care – and make changes to help prevent you from reaching the state of osteoporosis.
Treating Osteoporosis
There are a number of medical treatments that help you manage osteoporosis. These work by either slowing down the cells that break down bone, stimulating the cells that build new bone, or both.
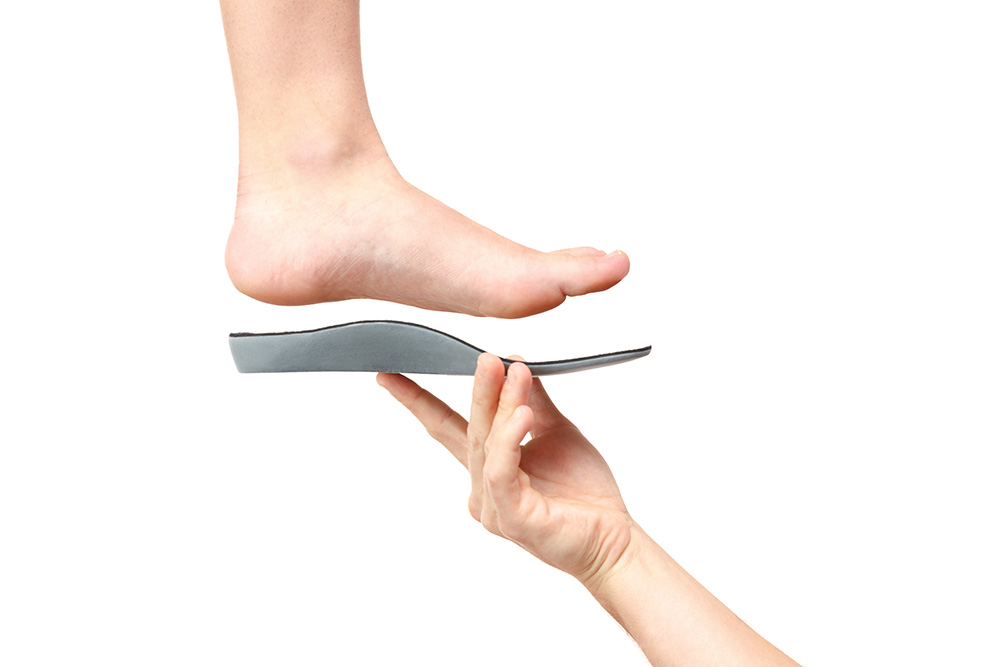
Here at My FootDr, we help patients affected by or at risk of osteoporosis by helping reduce their risk of falls and improving their stability and comfort on their feet. We can also identify areas of high stress that may be more vulnerable to fractures, and work to reduce the stress to these areas, and redistribute weight forces more evenly over the bones and joints. Custom foot orthotics are a great tool to help achieve these goals, as is physical therapy and footwear assessment.
Your personal risk factors, symptoms, history and your foot biomechanics are uniquely assessed at your appointment, so your podiatrist can create the right treatment plan for you to optimise your health and outcomes.