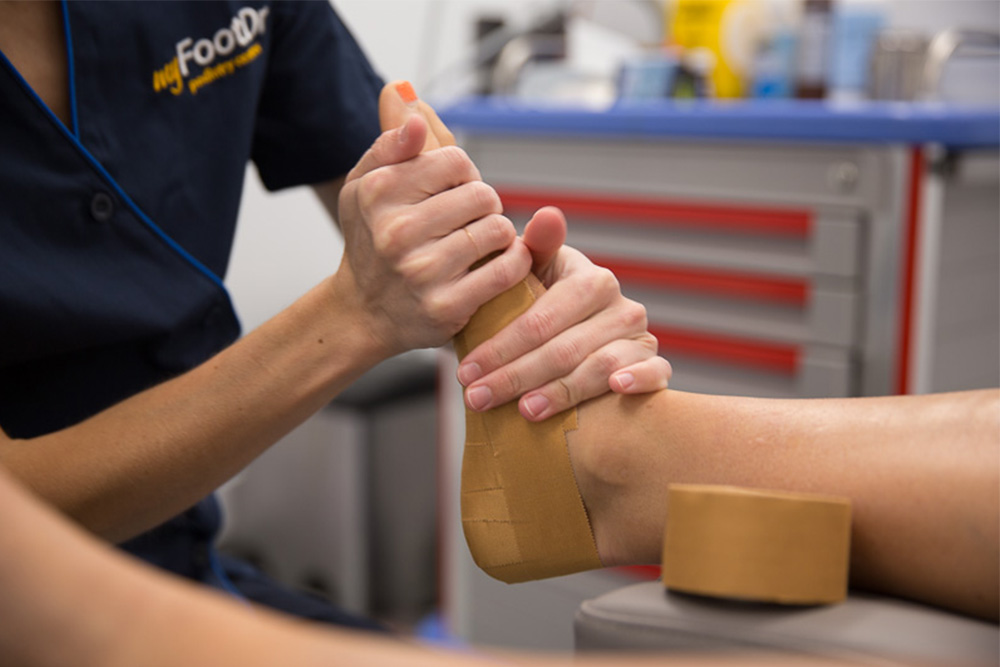
If you’re experiencing pain on the inside of your ankle, particularly just below that bony bump (your medial malleolus), then you may have irritated your posterior tibial tendon.
Your posterior tibial tendon is a fibrous cord which runs down the inside/back of your leg, beneath your ankle, and down into your arch. It plays a major role in helping us walk – without it, we’d struggle to stand on our tiptoes – and often do struggle when the tendon is injured.
When this tendon is injured, it is medically referred to as posterior tibial tendon dysfunction (PTTD).
What Causes PTTD?
PTTD is often an overuse condition. This occurs when heavy loads or excess strain is placed on the tendon, exceeding what it can safely handle. This overloading may be caused by:
- Your foot type and gait characteristics, especially flat (pronated) feet
- Regularly wearing unsupportive footwear
- Increasing the intensity of physical activities like hiking, running, long-distance walking and even climbing stairs
- Working on hard floors
- Increased weight, which may place more pressure on the tendon
The Symptoms
- Pain and tenderness on the inside of the shin, ankle or foot
- Swelling
- Muscle aches and fatigue in the affected area
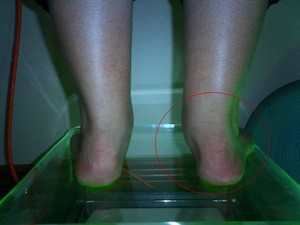
- Flattening of the affected arch (see below)
When the posterior tibial tendon is not functioning well, flattening of the foot can sometimes result, often referred to as adult acquired flat foot (AAFF).
The Pain Gets Worse Over Time
PTTD can be a progressive condition – the symptoms may worsen as the condition persists. This means that:
- When your symptoms first begin, you may feel pain on the inside of the foot and ankle (along the course of the tendon). The area may also be red, warm, and swollen
- As the condition worsens, your arch may begin to flatten. There may still be pain on the inside of the foot and ankle. At this point, the foot and toes begin to turn outward, and the ankle rolls inward
- When left untreated, the arch flattens even more and the pain often shifts to the outside of the foot, below the ankle. The condition may progress to a point where the tendon may tear completely
With appropriate and rapid treatment by your podiatrist, the progression of this condition can be slowed considerably. In some cases, it may cease completely. Depending on your stage of injury, your treatment can vary but will include one or more of the below:
- Short-term immobilisation with a moon boot or other device
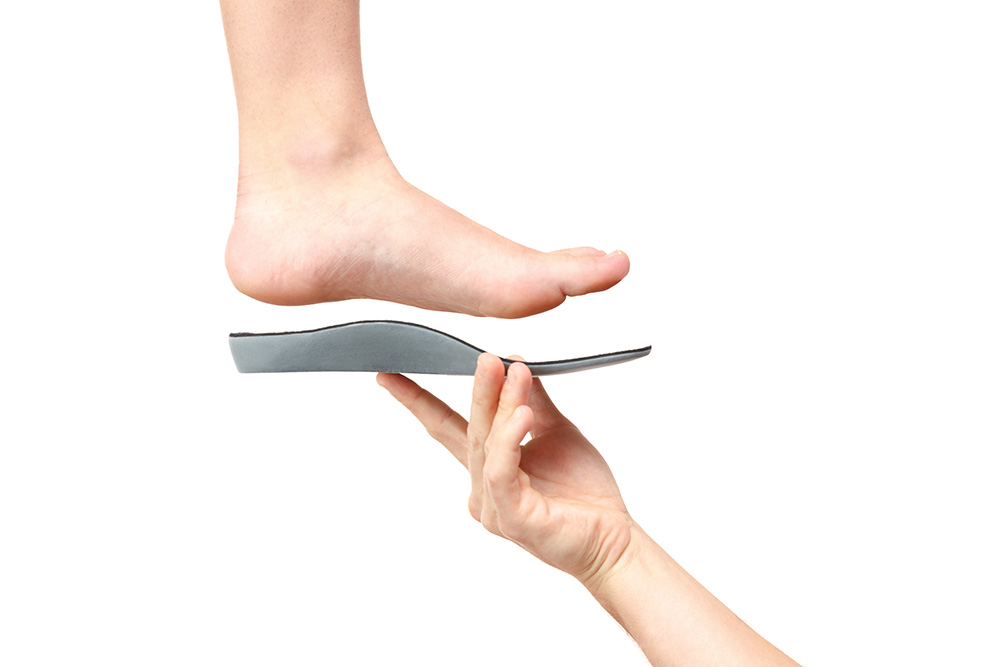
- Orthotics to provide support to the arch and tendon
- Above ankle articulation braces
- Shoe modifications, or new footwear recommendations
- Stretching and strengthening to help rehabilitate the surrounding musculature
- Medications
- Surgery, if indicated in the event that other alternatives have delivered suboptimal results