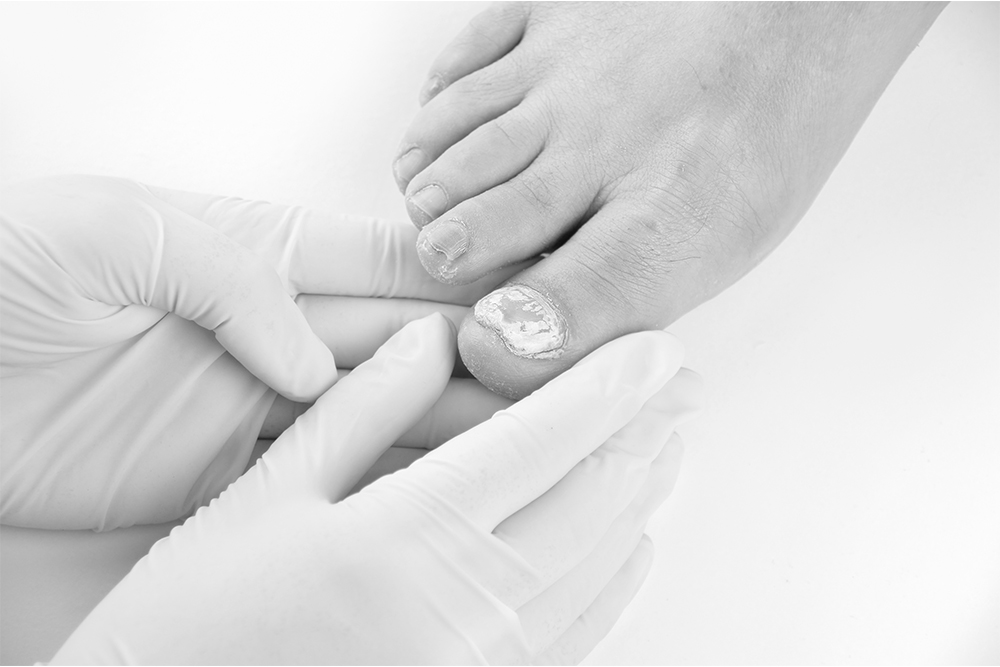
Fungal nail infections, medically known as onychomycosis, occur when a fungus comes in contact with and infiltrates a nail. These infections occur in both fingernails and toenails, and are more often seen on toenails because of the dark, warm and moist environments inside shoes, where fungus thrives.
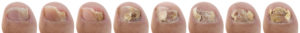
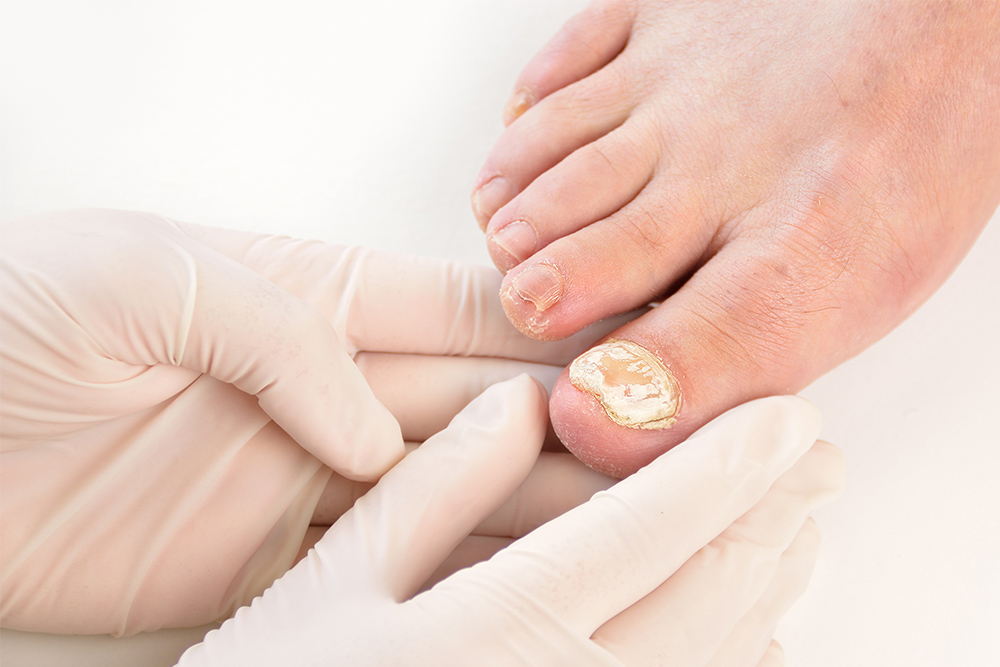
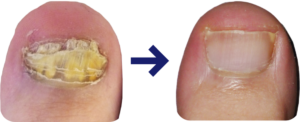
Fungal infections can cause the nails to thicken, discolour (yellow/white/brown), deform, crumble and split. We often see and treat fungal nail infections because patients are unhappy with the appearance of their nails, they don’t want them spreading to the other toes or to their family members, or the thickening nails have started to become painful.
Causes of Fungal Nails
When living fungus invades the nail through the nail bed or nail plate, it begins to feed on the keratin that comprises the nail, causing the changes in appearance. Not all nails that come in contact with a fungus will become infected, but it is more likely to if the nail is vulnerable, like when it has been damaged or a person’s immune system is compromised.
When an infection is superficial with only slight streaks or spots, it is the easiest to treat and completely eliminate the infection. As the infection spreads and starts growing beneath the nail, it is much more difficult to treat with traditional creams or lacquers, as they do not fully penetrate and reach all of the fungus. Any living fungus will continue to grow and spread. This is why we use deep-acting treatments like antifungal laser to clear fungal nail infections.
The primary types of fungi that cause fungal nail infections are dermatophytes, but other fungi such as yeasts and moulds may also be the culprit. As these fungi thrive in a warm and moist environment, common sources of infection come from sharing showers, public changing rooms and pools, and sharing socks and shoes.
There are several factors that may put you at increased risk of developing fungal toenails. These include:
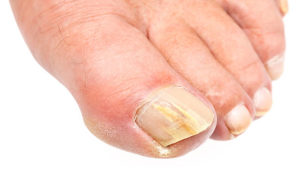 Trauma to the nail, like from repetitive rubbing against the toes, or a one-off injury like stubbing your toe
Trauma to the nail, like from repetitive rubbing against the toes, or a one-off injury like stubbing your toe- Poor hygiene – not drying off the feet thoroughly after showering or exercise
- Excessive sweating
- Having a compromised immune system – including people with diabetes and HIV
- Poor peripheral circulation
- Wearing occlusive footwear like boots or sneakers daily
- Working in a wet environment
Typical Demographic
Toenail fungus is rare in children but the incidence increases as you age. This condition is most common in people aged over 60 years.
Diagnosis of Fungal Nails
Several nail disorders may look like fungal nail infections, including psoriasis. This is why it’s important to get an accurate diagnosis from your podiatrist, so you don’t waste time and money on treating the wrong condition. Our qualified podiatrists can diagnose a fungal infection from a physical examination, and if needed, we can have a sample of the nail tested by a lab to confidently confirm the diagnosis.
Treatment
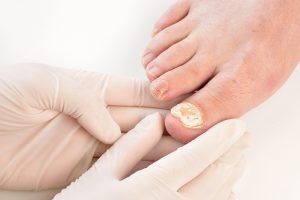 Treatment options for fungal nail infections include topical medications, oral medications, and medical laser treatment. Any treatment will help destroy the living fungus, but it won’t reverse the damage that the fungus has already inflicted on your nail. If you’d like to restore the appearance of your nail as well as treating it, opt for keryflex nail restoration alongside your antifungal treatment.
Treatment options for fungal nail infections include topical medications, oral medications, and medical laser treatment. Any treatment will help destroy the living fungus, but it won’t reverse the damage that the fungus has already inflicted on your nail. If you’d like to restore the appearance of your nail as well as treating it, opt for keryflex nail restoration alongside your antifungal treatment.
Laser Treatment
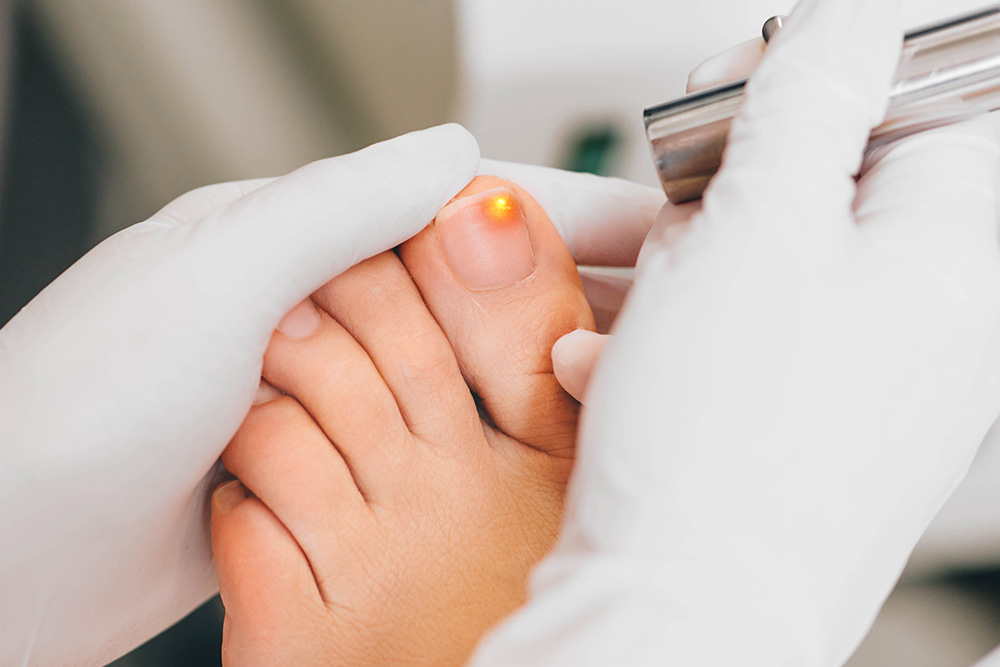
Laser is a major advancement in the treatment of fungal nail infections with an over 80% success rate, as published in clinical trials. Laser light is used to penetrate the nail plate, destroy the fungus in a series of treatments without damaging the nail or the skin around it. The procedure is pain-free and there are no side effects. After the treatment, the nail is able to grow out free of infection.
Laser is our number one recommended anti-fungal treatment.
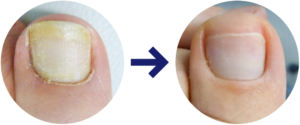
Topical Medication
A medicated nail lacquer is applied to the nails daily for a long period, often multiple times per day. There are no side effects, although you must take care to avoid the lacquer touching the surrounding skin, as this can cause irritation. Applying these lacquers and creams is a laborious task and many people struggle to keep it up, especially as you don’t see any instant results. This treatment is not suitable for anyone that struggles to reach their feet.
While this option has a generally low cost, it has low success rates in clinical studies of 8-10%. This is likely because the medication doesn’t readily penetrate into the nail plate or nail bed to reach all of the fungi.
Oral Medication
Tablets can be taken orally for approximately 6-12 weeks. Clinical studies have shown oral medications to yield better results that topical lacquers, but not to be as high as laser treatment. This medication must be prescribed by your doctor, and blood tests may be required to ensure your liver is functioning properly; blood chemistry is often monitored quarterly for those at risk of adverse effects such as liver disease.
The success rate is approximately 50%, however, they are significantly more costly than lacquers and side effects are well documented in a number of people who take these oral anti-fungal medications.