Metatarsalgia is a broad term that describes pain in the forefoot, in the area of the metatarsal bones. These are the long bones in your forefoot that connect to the toes. There are five metatarsal bones in each foot and they play an important role in helping you push off against the ground during walking and running. The anatomy of the forefoot is quite complex and there are numerous joints, ligaments, muscles and nerves that may be the source of pain in this area of the foot.
The Cause Of Metatarsalgia
As metatarsalgia is a broad term describing pain in the forefoot, there may be many sources of pain in this region. Your podiatrist will perform a thorough physical examination to determine the structures involved and identify the source of your pain.
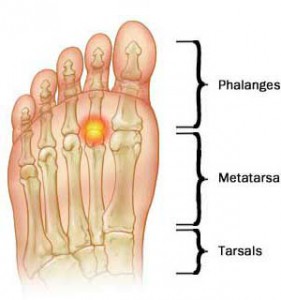 Metatarsalgia may be related to:
Metatarsalgia may be related to:
- Joint inflammation
- Nerve compression or aggravation
- Plantar plate (ligament) tear
- Bursitis
- Bone stress injury
- Arthritic conditions
Contributing factors may include:
- Increasing the intensity or duration of physical activity in a manner that your body is not accustomed
- Foot structure and function – the shape of our bones and joints, as well the way they move, can contribute to altered loading in the forefoot
- Footwear – poorly fitting footwear (too narrow through the forefoot) or footwear that is worn out can also alter loading through the forefoot.
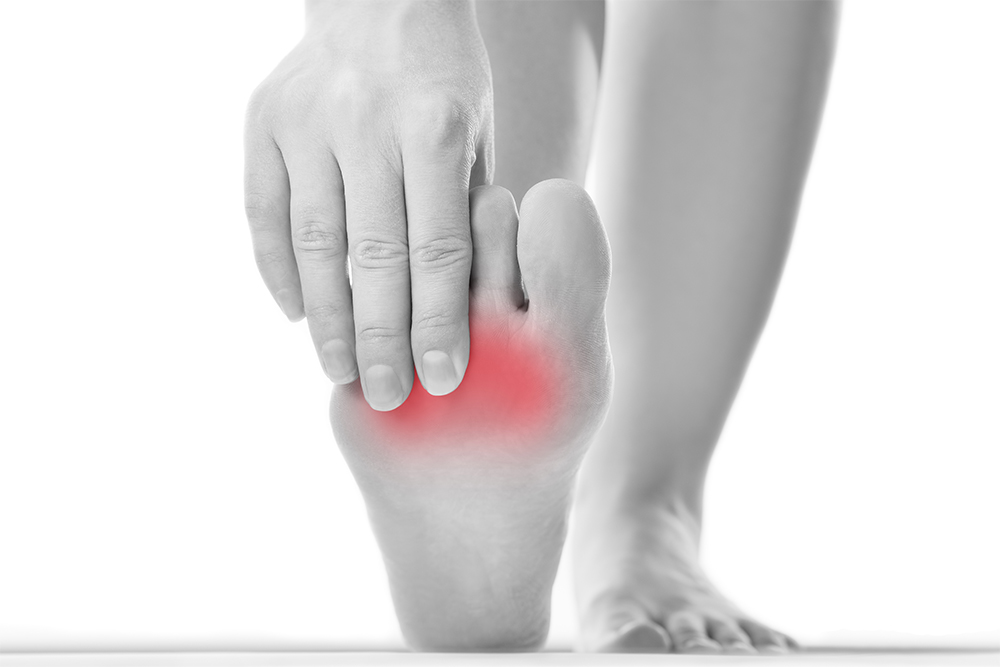
Metatarsalgia Symptoms
- Pain at the ball of the foot (at any one of the five joints)
- Pain on the top of the forefoot
- Tenderness to touch
- Burning or throbbing feeling around the bony part of the ball of the foot
- Shooting pains that extend into the toes
- Numbness or pins and needles in the toes
- Pain that is exacerbated by standing, walking or running
Managing Metatarsalgia
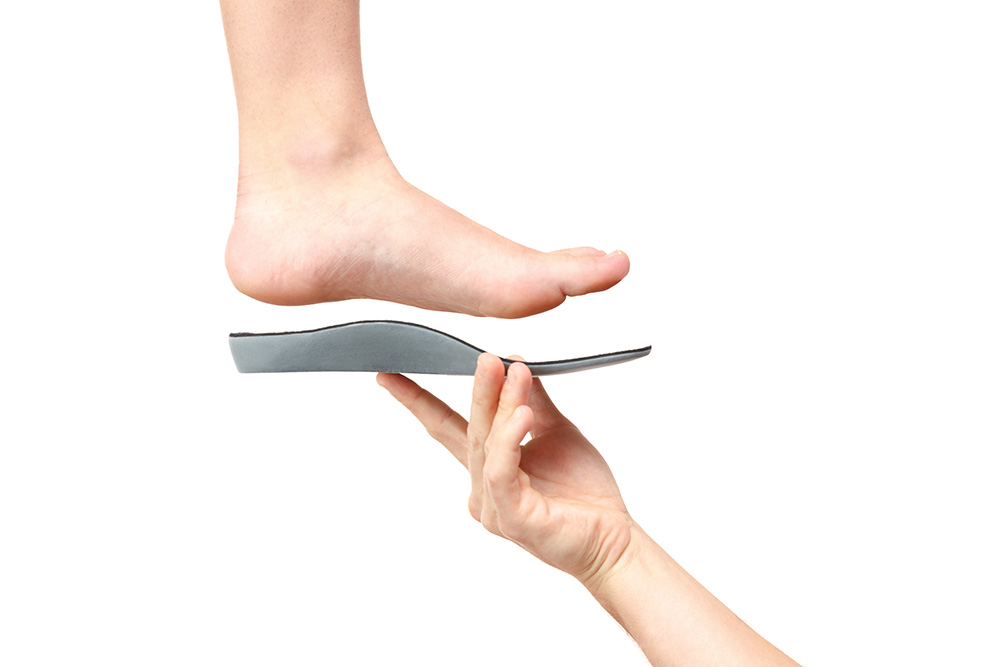
As there are many different conditions that may produce metatarsalgia, an accurate clinical diagnosis is an important step to ensure you receive the correct treatment. Your podiatrist will perform a thorough physical assessment of the painful site, accompanied by a detailed discussion with you, to understand how the pain started and the history of your symptoms. Your podiatrist will develop a treatment solution that is tailored to your specific diagnosis, with consideration for contributing factors such as your level of physical activity, your individual foot structure (bony alignment) and also your foot biomechanics (the way your feet move). Common treatment approaches include modification of weight-bearing activities, footwear advice, foot orthoses, as well as strength and mobility exercises.
Before you come in to see your podiatrist, you can rest from aggravating activities, use ice for relief of pain and inflammation, and if necessary, seek advice from your pharmacist about non-steroidal anti-inflammatories like ibuprofen. This is not a long-term solution, however, as the symptoms will likely return when you resume walking.