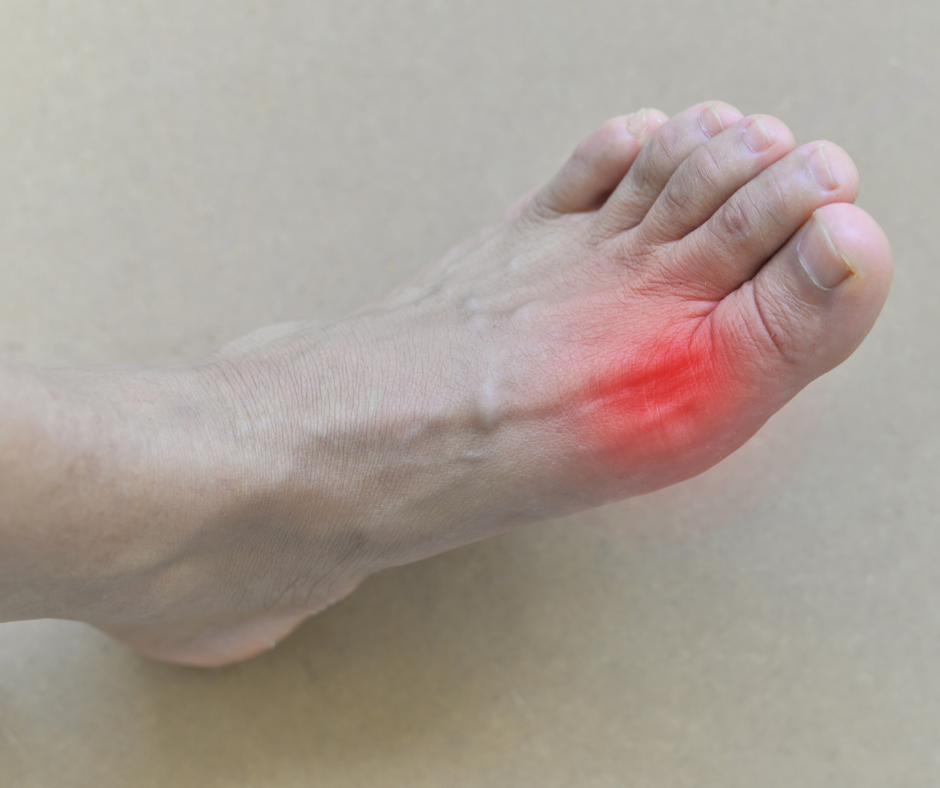
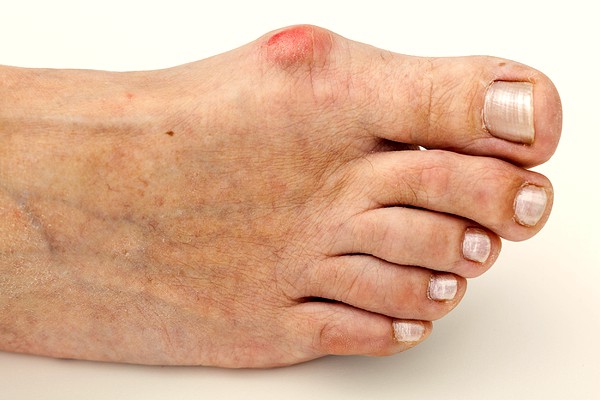
Osteoarthritis is best known as the wear and tear arthritis that is a common cause of joint pain and mobility restrictions in older adults. Traditionally, osteoarthritis was thought to be related to the gradual wearing down of the cartilage that covers the ends of the bones within a joint. In recent years, this has been redefined to include that all of the components of the joint are involved alongside the thinning of the cartilage, including the joint lining, ligaments, bones and muscles. It also appears that the body’s response in actively working to repair the joint damage can result in or contribute to the structural joint changes in osteoarthritis that can restrict movement and cause pain.
Osteoarthritis is best known as the wear and tear arthritis that is a common cause of joint pain and mobility restrictions in older adults. Traditionally, osteoarthritis was thought to be related to the gradual wearing down of the cartilage that covers the ends of the bones within a joint. In recent years, this has been redefined to include that all of the components of the joint are involved alongside the thinning of the cartilage, including the joint lining, ligaments, bones and muscles. It also appears that the body’s response in actively working to repair the joint damage can result in or contribute to the structural joint changes in osteoarthritis that can restrict movement and cause pain.
Osteoarthritis can affect any joint in the body but often impacts our knees, feet and hips because of how much we use them and the force they take on in everyday life. While it’s more common in older adults, approximately 2.5% of the total arthritis sufferers (3.6 million Australians) are aged below 45 years.
What Happens In Osteoarthritis & Who Is At Risk?
Given that we all use our joints daily to stay mobile and active, no one is exempt from the risk of developing osteoarthritis. With this said, some factors are well-known to increase your risk. These include:
- Age – the prevalence of arthritis increases greatly with age
- Gender – arthritis is more common in women than men
- History of injury – if you’ve previously injured a joint or had surgery, it is more likely to develop osteoarthritis
- Genetics – some specific genes are identified that increase your risk of arthritis. One of these genes causes a mutation in our collagen
- Natural joint differences – some natural variances in joint shape or structure can predispose you to developing osteoarthritis
- Weight – given that weight is directly correlated to the pressure through our joints when we move, being overweight can place you at a higher risk of developing osteoarthritis
- Overuse – if you’re performing the same movements that load your joints day in and day out, like at work, you may be more likely to develop osteoarthritis
When our joints are healthy, all of the components of the joint work together smoothly to create frictionless, pain-free movement – from the cartilage that provides a slippery surface on our bone ends so the bones can glide smoothly past one another, to the synovial fluid and lining. When a joint starts becoming affected by arthritis, not only does that cartilage thin and the surface of the bones become rougher, but the body’s repair process can cause further structural changes to the joint itself, affecting all of its components. The capsule can thicken and stretch, the synovium can thicken and become inflamed, and bone spurs can develop within the joint.
Signs & Symptoms Of Osteoarthritis
 Joint pain and stiffness are the primary symptoms, and the severity of these can vary greatly from person to person and even week to week. Your joint may start to creak, and you may notice that your flexibility is reduced. Your joints may swell at times, and over time the shape and appearance of the joint may change. Many people with osteoarthritis report that factors like colder weather – and even the time of day – can affect the severity of their symptoms.
Joint pain and stiffness are the primary symptoms, and the severity of these can vary greatly from person to person and even week to week. Your joint may start to creak, and you may notice that your flexibility is reduced. Your joints may swell at times, and over time the shape and appearance of the joint may change. Many people with osteoarthritis report that factors like colder weather – and even the time of day – can affect the severity of their symptoms.
Diagnosing osteoarthritis is not difficult – it’s a combination of your symptoms paired with confirmation of the changes to the joint using medical imaging. The sooner you get a diagnosis, the sooner you can start taking the right steps to improve your comfort and help reduce the long-term consequences of arthritis on your body.
How To Treat Osteoarthritis
Once the changes to the integrity and structure of your joint begin, these are generally irreversible. With this said, osteoarthritis is a gradual process that worsens over time, and there is plenty that can be done to both slow the progression and help manage any painful symptoms, keeping you feeling more comfortable, supported on your feet, mobile, and independent. For arthritis impacting your feet and legs, these include:
- Footwear – don’t worry, you don’t need to change into large, clunky shoes. What your shoes must do is best support your foot posture, offload any prominent or painful joints, cushion the feet to better distribute pressure and forces when you walk, and accommodate any other problems like bunions
- Custom foot orthotics – we use orthotics to help our patients make significant improvements to their comfort and movement. Each pair is prescribed following a comprehensive assessment with your podiatrist, who understands the unique structural and functional needs of your feet. Our orthotics are designed using a 3D scan of your feet – so absolutely no ‘guesswork’ – and we adjust them to fit perfectly into your footwear
- Physical therapy – low-impact strengthening and stretching exercises are used to help you maintain your joint function, strength and flexibility
- Activity modification – depending on the severity of your symptoms, we may make recommendations to your regular activities to help slow down the progression of arthritis. If going for long walks is causing you pain, we may suggest shorter walks paired with pool-based exercise given the significant load reduction on your joints in water