
Are you one of the 48% of Australians that wakes up with heel pain once a week?
If heel pain is impacting how you move, how you feel, and how you live, then it’s time to get help from My FootDr.
Heel pain, often caused by plantar fasciitis, is a common condition that can cause severe pain at the bottom and inside of the heel. This pain may radiate up into the arch, and indicates that there is some damage to, and subsequent inflammation of, the long band of tissue under the foot known as the plantar fascia.
Damage to the fascia usually starts with micro-tears and progresses to partial tears across the tissue. At its worst, the fascia may completely rupture. Early diagnosis and treatment can prevent this injury from progressing to be a longstanding and ongoing problem (chronic), which is when pain relief, walking, and normal everyday activities become much more difficult.
Here at My FootDr, our podiatrists use a best-practice approach to treating plantar fasciitis that combines proven treatments with what gets the best results for our patients. Every treatment is tailored to each person based on the severity of your plantar fasciitis, your current symptoms and your daily life, but may involve:
- Shockwave therapy
- Custom foot orthotics
- Strapping or bracing
- Specific exercise prescriptions (both strengthening and stretching)
- Footwear recommendations
My FootDr’s Top Tips For Healthy Heels
1. Always get a diagnosis from a podiatrist that specialises in heel pain
You trust your dentist with your teeth and you can trust My FootDr’s team of highly-qualified podiatrists to care for your feet. Our podiatrists always provide that extra level of care and attention when delivering the best in foot care solutions for heel, arch, and foot pain caused by plantar fasciitis.
Our experience in treating heeling pain means that we can differentiate between plantar fasciitis and other causes of heel pain including abductor hallucis tendinopathy, stress fractures, plantar fat pad atrophy, and more. We’ll then get your treatment underway promptly to help you get the best outcomes for your foot pain.
2. Take steps to minimise pain, and rest
Until you make it in to see your podiatrist, make sure to rest your injured foot, keep it elevated, and use ice for approximately 20 minutes at a time using a towel or cloth so that the ice isn’t applied directly to the skin.
Once you make it in to see your podiatrist, they may use some temporary measures to help relieve your pain and discomfort like strapping the heel, and teaching you how to replicate this strap at home.
3. Technique matters
Stretching and strengthening exercises can be helpful in heel pain treatment and rehabilitation, but, only if performed correctly and at the right time.
Stretching and strengthening addresses any existing muscle imbalances, such as tight and weak muscles. This can help decrease the chance of re-injuring your heel in the future, as well as reducing your current symptoms.
Morning stretches before you get out of bed can help reduce the intensity of your pain during those first few steps. Your podiatrist will prescribe a specific stretching and strengthening program to suit you.
If you need additional short-term relief, ask your podiatrist about our shockwave treatment.
4. Choose the right footwear for your feet
The right footwear should provide the right balance between support and cushioning. Your podiatrist will provide footwear recommendations to suit your condition, level of activity and foot type. Without the right footwear helping to support your foot and ankle, you risk prolonging your recovery.
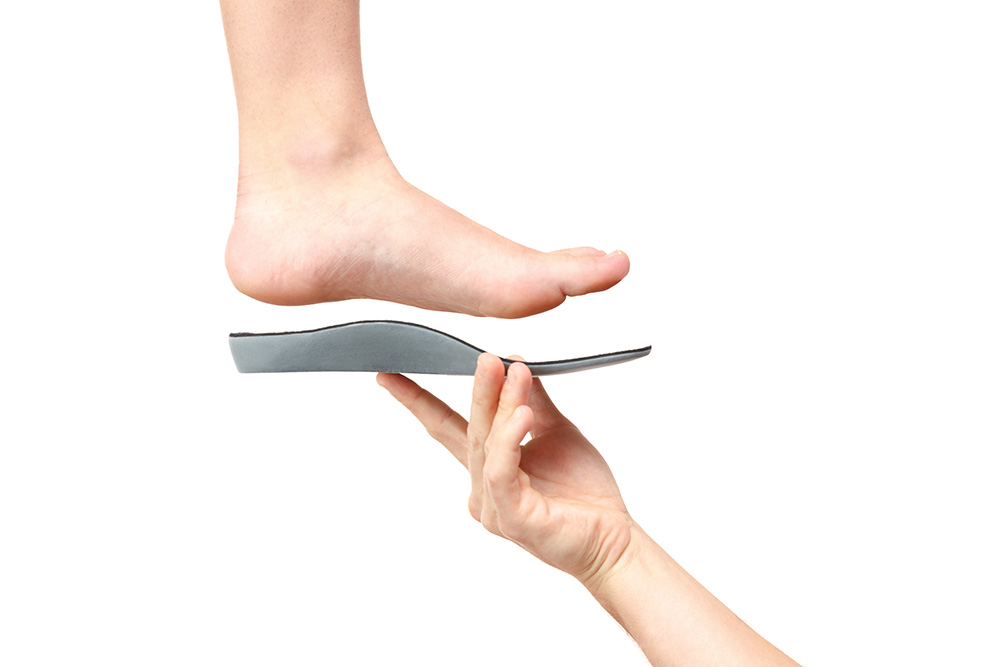
5. Wear custom foot orthotics if prescribed by your podiatrist
A biomechanical assessment performed by your podiatrist will determine whether you need orthotics – both to help you recover and prevent the problem from recurring by keeping your feet well-supported. Custom-made orthotics will offload the damaging forces away from the heel and fascia, allowing it to heal and helping prevent heel pain. Orthotics will also help to support your feet and legs whenever you’re on your feet. This improves your foot and leg function, weight distribution and posture, assisting with a range of problems and generally helping you to move with greater comfort.
6. Commit to an annual check-up
Our feet and legs change over the years, and our shoes and orthotics wear down over time. Committing to an annual (or as recommended) check-up with your podiatrist means that problems can be identified and addressed before they become painful, keeping your foot health a priority, and helping to prevent plantar fasciitis from starting or returning.