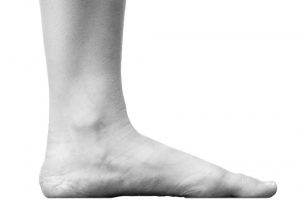
What Are Flat Feet?
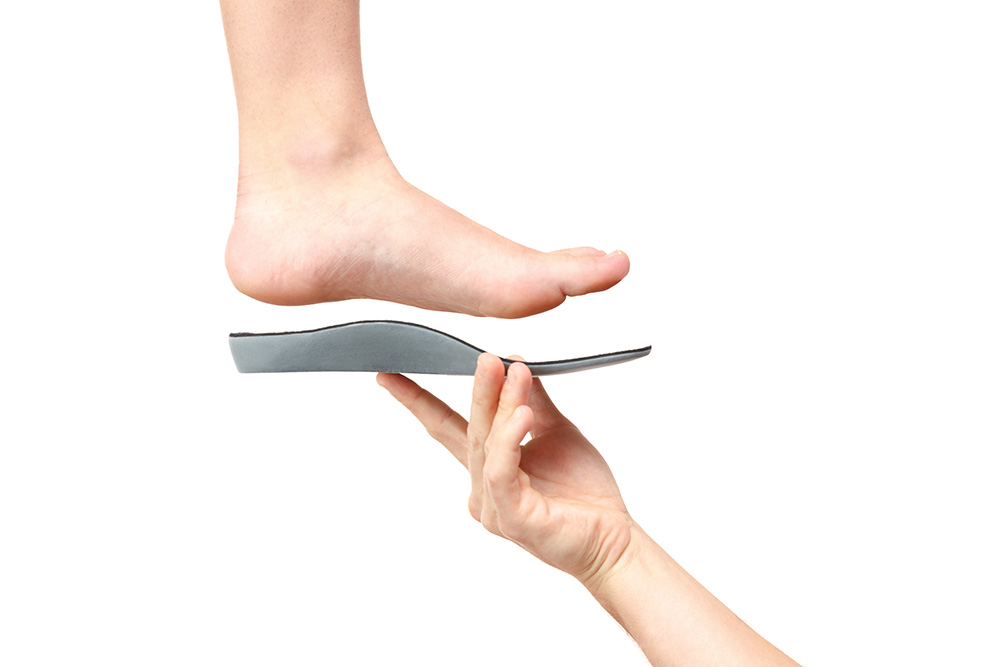
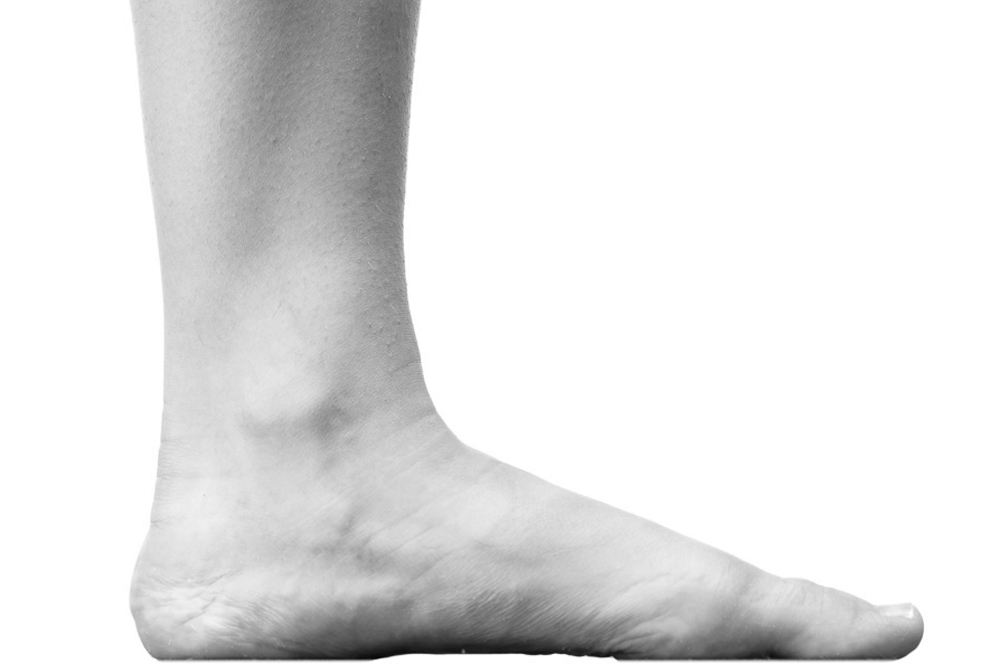
If your feet appear to have no arch and excessively roll inwards and downwards towards the floor when you’re standing, then it’s likely that you have flat feet.
Even though your feet may appear to have a well-defined arch when you sit and have your foot off the ground, it’s the position when we’re standing that we are most interested in. This is because this inwards rolling, known as pronation, can sometimes place excess stress on muscles, tendons, ligaments and bones in the feet, making you more vulnerable to foot pain.
What Causes Flat Feet?
There are many causes of excess pronation, including:
- Hypermobility. This describes excess laxity in the tissues and ligaments which makes you more flexible. The same applies to the ligaments in the feet, hence leading to pronation. This is present in approximately 10% of the population
- Soft tissue injury, e.g. posterior tibial tendon dysfunction
- Hereditary bony or soft tissue conditions within the foot that disrupt normal walking patterns. This causes the foot to “unlock”, allowing the arch to fall closer to the ground
- Abnormal muscle length or weak muscles
- Pregnancy and hormonal changes
- Medical conditions including arthritis and diabetes
- Abnormal leg rotations
- Leg length difference
- Spinal conditions, e.g. scoliosis
- Muscle spasticity, e.g. Cerebral Palsy
The result of pronation can vary from patient to patient. While some people may remain asymptomatic, for others the abnormal force from the effects of pronation on the body can be a major contributor to a myriad of bony and soft tissue problems, often leading to pain.
Flat Foot Symptoms
When flat feet or pronation forces become excessive or abnormal, symptoms may occur in the following areas:
- Feet (e.g. bunions, hammertoes, corns, calluses)
- Heels (e.g. plantar fasciitis, heel spurs, heel pain, Sever’s disease)
- Shins (e.g. shin splints, posterior tibial tendinopathy, PTTD)
- Knees (e.g. patellofemoral syndrome, chondromalacia (runners knee), Osgood Schlatter’s disease
- Thighs (e.g. Iliotibial band syndrome)
- Hips (e.g. greater trochanter bursitis)
- Upper and lower back (e.g. sciatica, disc protrusion)
- Neck and head secondary to poor postural alignment which can occur with kyphosis
You may also notice that your shoes wear out faster on the inside edges, and you may observe some ‘bulging’ on the inside of your ankle.
How to Cure and Treat Flat Feet
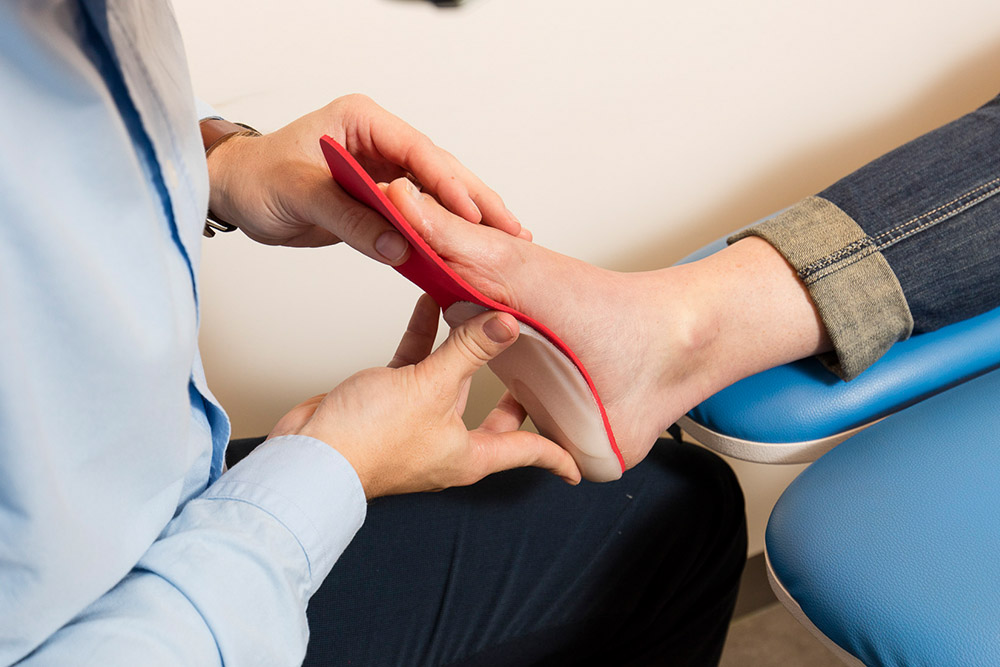
At My FootDr, our podiatrist will carry out a detailed biomechanical assessment of your feet, legs, knees and hips to identify the cause.
An analysis of your walking pattern with computerised video gait analysis software is performed to assess the effect on your gait. Your Podiatrist will then discuss your treatment options which will often include a pair of custom foot orthotics to control any abnormal forces causing any associated foot pain, leg pain or other symptoms.
A 3D scan of your feet is taken and a detailed prescription is created for you, from which a pair of orthotics can be made. Your orthotics are designed to fit inside your footwear comfortably to support your arch and feet in their most optimal position. This is to help your alignment and posture, and relieve some strain away from overused muscles.
Your podiatrist will also make a recommendation on the best footwear for your feet, and ensure that your current footwear is suitable, and is not hindering your recovery. This is important as footwear has the ability to help support and stabilise our feet, improving their efficiency and the way we are using our muscles, joints, bones and ligaments.
Your treatment plan is always completely tailored to your symptoms and what has caused your flat feet. Your treatment may also involve exercises, mobilisation, manipulation, massage, footwear advice, postural balance programs, dry needling, and in some cases, shockwave therapy. All of these options will be discussed with your Podiatrist if they feel you require this treatment.
Flat Feet FAQs
Are flat feet permanent?
In most cases flat feet are permanent, but that doesn’t mean that they have to cause you pain and discomfort. Most people are able to live a happy, active and pain-free life without flat feet holding them back or causing problems, by having the right support and care for their feet.
Is walking barefoot good for flat feet?
No, generally not. As your muscles and tendons must often work harder with every step when you have flat feet, walking with bare feet and without support exacerbates this, making you more likely to develop tired and achy legs, if not more serious problems.
How to relieve pain from flat feet
It’s not the foot type itself that is producing pain, but specific muscles and tissues that are overworking and becoming strained. Effectively relieving pain means identifying and addressing these specific structures. This may be as simple as using strapping tape temporarily, custom-foot orthotics for long-term relief, or treating any injuries that have developed which may use shockwave or other suitable treatments. Relieving pain from flat feet must be done on a case-by-case basis, specific to which structures in your feet are now injured.
What kind of shoes are good for flat feet?
Shoes with in-built arch support are a good start for flat feet. The shoes should help support the foot while keeping the foot and ankle stable. They should also be matched to your activity – whether that be exercise, work, or daily life. Ideally, the shoes should wrap around the ankle for best support, and have good fastening mechanisms. Your My FootDr podiatrist can make the best recommendations for your specific circumstances and foot characteristics – and we have a wide range available at both our retail centres and online.