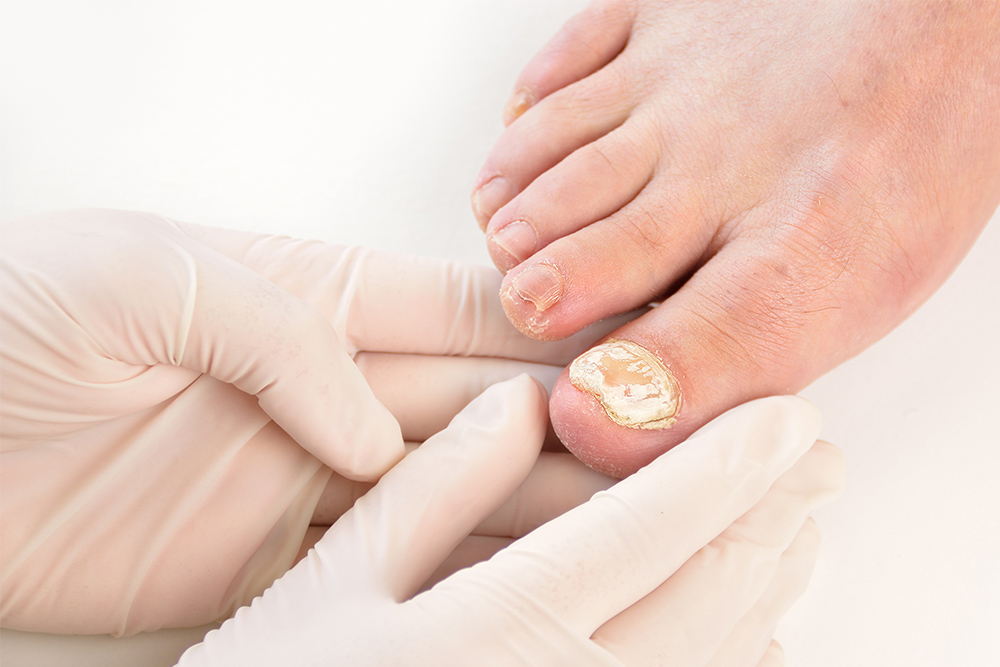
Onychomycosis is a word that has probably never been used in your household before. As the medical name for fungal nail infections, it might also not be something that gathers much airtime at the family dinner table either. However, while some people may feel embarrassed revealing such a foot condition, there really is nothing taboo about talking about toenails.
Onychomycosis is a word that has probably never been used in your household before. As the medical name for fungal nail infections, it might also not be something that gathers much airtime at the family dinner table either. However, while some people may feel embarrassed revealing such a foot condition, there really is nothing taboo about talking about toenails.
What causes fungal nail infections?
As you get older the incidence of fungal nail infections increases, so it’s important that we all know what it is and how to treat it.
Onychomycosis is caused by fungal organisms that invade the nail through the nail bed or nail plate. The nail itself provides a protective covering that allows the fungus to grow underneath on the nail bed unimpeded.
The primary fungi that cause onychomycosis are dermatophytes, but non-dermatophyte fungi such as yeasts and moulds may also be causative agents. These fungi thrive in a warm and moist environment.
What factors can contribute to fungal nail infections?
Fungal nail infections typically develop over time and it can be difficult to notice any immediate difference in the way your toenail looks or feels. However several factors can put you at an increased risk of developing the condition.
Some of these include:
- Nail trauma – acute or repetitive micro-trauma such as rubbing
- Poor hygiene – not drying off the feet thoroughly after showering or exercise
- Living in a warm, humid environment
- Excessive sweating
- Having a compromised immune system – including people with Diabetes
- Poor peripheral circulation
- Warm, moist environment from enclosed footwear
- Working in a wet environment
Diagnosing and treating the condition
Our Podiatrists perform a physical examination and in some cases a microscopy and/ or culture of nail specimens if required.
Adam Preston, our Podiatrist from My FootDr Currambine and West Perth, says because most treatments rely on reducing the spread of the fungus and waiting for the nail to slowly grow out, traditionally it can take a long time to get on top of the condition.
“Topical and oral treatments have been used to treat fungal nail infections for years, but they have a relatively low strike rate,” he says.
“However, we are now focusing on laser treatment which has been a huge advancement in treating fungal nail infections in recent years.”
He says laser treatment for fungal nail infections was a far more effective treatment option for patients.
“At My FootDr Perth and Currambine we use the lunula cold laser, which penetrates the nail and destroys the fungus in a single treatment without damaging the nail or skin itself – and most importantly without any pain or side-effects.”
“The success rate of topical and oral medication can be as low as 10% and 50% respectively – and some patients experience other side-effects from oral medication. Fungal nail laser treatment is effective in 80% of cases.”