

Diabetes is a disorder that affects the entire body – including having severe consequences for the feet.
How diabetes affects your feet and body
Overall, diabetes impairs the body’s ability to absorb sugar (glucose) from the bloodstream and provide it to the tissue cells that need it for normal activity and health. This results in high levels of glucose remaining in the bloodstream and producing toxins that affect all body organs and systems, including the circulatory system and the peripheral nerves in the feet and legs.
In simple terms, diabetes impairs your circulation, your protective sensation (ability to feel) in your feet and legs, and your ability to fight infection due to an impaired immune system. Diabetes does not affect everybody in the same way or with the same severity, but the symptoms do tend to progressively worsen over time. Research has shown that strict adherence to medical treatment and regular exercise helps to stabilise blood glucose levels and is, therefore, the best way to avoid these complications.
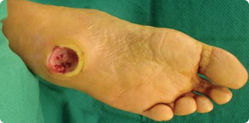
Symptoms affecting your feet and legs
Initially, changes may be minimal such as noticing dryness of the skin around the toes, or tingling of the toes at night. Eventually, this may progress to complete numbness along the sole, which makes you unable to detect any cuts or damage to the feet. When you don’t know that damage has occurred, you don’t realise that you need any treatment, and you become vulnerable to infection of an untreated wound.
Reduced circulation (blood flow) to the feet and lower limbs means your tissues receive less oxygen and nutrients. This means that your body’s ability to repair any damage, heal any cuts and fight infection is impaired. This is why diabetes is the leading cause of lower limb amputation in Australia, aside from trauma.
Reducing your risks and managing your foot health
Diabetes Australia recommends an annual check by a qualified podiatrist to assess your foot health. As the status of your foot health changes over time, so does the advice around the precautions you should take. As skilled professionals in this field, podiatrists use diagnostic tests to assess your sensation, circulation and biomechanical risk factors, and consider the results of these tests within the bigger picture of your overall health. Information on what to expect during your annual appointment and Frequently asked questions can be found below.
What to expect from your Diabetes Foot Check?
The appointment for your Diabetes Foot Check will be broken out into 5 parts: nerve review, blood flow test, skin and nail check, foot movement/joints and footwear.
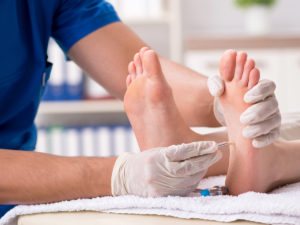
1. Nerves
- To test the feeling in your feet a fishing line wire-like tool or a vibration device is used
- To check your muscles are working, you will be asked to push your feet against the podiatrist
2. Blood Vessels
- A Doppler ultrasound device should provide a review of the amount of blood flow is coming to your feet or the Podiatrist should use their fingers to check your pulses.
3. Skin and Nail
- To check your nails for any signs of infection, thickness that can damage your skin and other issues that affect your skin health like callus and corns.
- The skin will be also checked for any trauma like cuts and bruises or sores.
4. Foot Shape/Movement and Footwear
- To check how you move your feet and how the muscles around your feet and ankles are working.
- Will check your shoes and ask you about your footwear habits.
Questions your Podiatrist may ask you:

- Have you ever had a foot ulcer?
- Have you seen any cuts or blisters that you did not feel?
- Do you notice any discomfort through the day or at night?
- If you do have pain, does anything help it?
- Do you check your feet daily?
- How has your diabetes been lately?
Questions to ask your Podiatrist:
- What is my foot health risk factor?
- What advice can you give to care for my feet – according to my level of risk?
- What is the proposed treatment plan?
- Do I need to be referred to a specialist for expert advice?
Click book now to schedule an appointment at your nearest My FootDr Clinic.
Tips to help maintain your foot health
- Wash feet and dry feet thoroughly every day, making sure to dry well between the toes
- Look over your feet every day to check for any marks, spots, cuts, swelling or redness that is not normal. If you have difficulty getting your leg up to see the sole of your foot, use a mirror to help. If you notice anything that may be concerning, let your Podiatrist or GP know immediately
- Choose correctly fitted shoes with adequate depth and width for the toes. This minimises your risk of damage to your feet
- Opt for cotton socks with no elastic in the tops, as they will absorb sweat and reduce pressure at the top of the sock line
- See your podiatrist every year for a diabetic foot assessment
Having regular foot care from your podiatrist plays an integral role in the prevention of diabetic foot complications, and has been shown to decrease the likelihood of a diabetes-related amputation.
In addition to regular podiatry assessment and treatment, you can do these simple things at home to take care of your feet.
- Never walk barefoot
- Cut your toenails straight across carefully with good quality nail nippers and file afterwards
- Moisturise your feet daily but avoid moisturising in between your toes
- Have any corns and calluses treated by a podiatrist. Never use over-the-counter corn pads or razor blades
- Check the inside of the shoes for foreign objects before you put them on
- Keep your feet away from direct heat including heaters, hot water bottles, scalding hot showers/baths and electric blankets
- Enjoy exercise and try to be generally active while taking care to prevent injury

